|
|
What Is Back Pain?
Back pain is an all-too-familiar problem that can range from a dull,
constant ache to a sudden, sharp pain that leaves you incapacitated.
It can come on suddenly – from an accident, a fall, or lifting
something too heavy – or it can develop slowly, perhaps as the
result of age-related changes to the spine. Regardless of how it happens
or how it feels, you know it when you have it. And chances are, if
you don't have it now, you will eventually.
How Common Is It?
At some point, back pain affects an estimated 8 out of 10 people.
It is one of our society's most common medical problems.
What Are the Risk Factors for Back Pain?
Although anyone can have back pain, a number of factors increase
your risk. They include:
-
Age: The first attack of low back pain
typically occurs between the ages of 30 and 40. Back pain becomes
more common with age.
Fitness level: Back pain is more common
among people who are not physically fit. Weak back and abdominal
muscles may not properly support the spine. "Weekend warriors"
– people who go out and exercise a lot after being inactive
all week – are more likely to suffer painful back injuries
than people who make moderate physical activity a daily habit.
Studies show that low-impact aerobic exercise is good for the
discs that cushion the vertebrae, the individual bones that make
up the spine.
Diet: A diet high in calories and fat,
combined with an inactive lifestyle, can lead to obesity, which
can put stress on the back.
Heredity: Some causes of back pain,
including disc disease, may have a genetic component.
Race: Race can be a factor in back
problems. African American women, for example, are two to three
times more likely than white women to develop spondylolisthesis,
a condition in which a vertebra of the lower spine – also
called the lumbar spine – slips out of place.
Side View of Spine
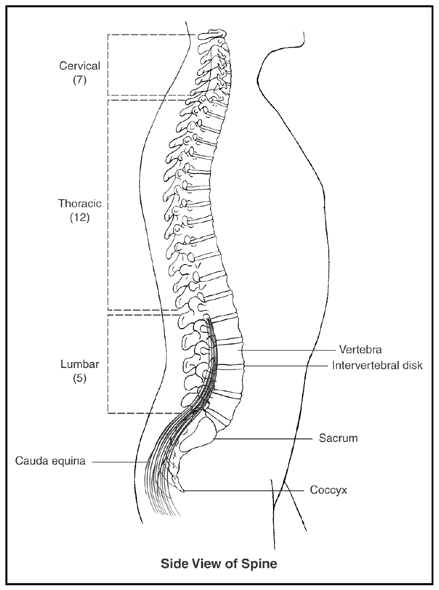
Normal Vertebra
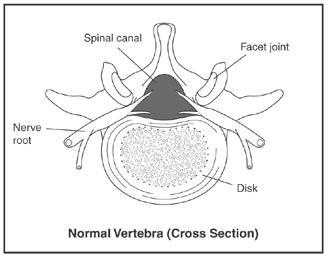
The presence of other diseases: Many
diseases can cause or contribute to back pain. These include various
forms of arthritis, such as osteoarthritis, rheumatoid arthritis,
and ankylosing spondylitis, and cancers elsewhere in the body
that may spread to the spine.
Occupational risk factors: Having a
job that requires heavy lifting, pushing, or pulling, particularly
when this involves twisting or vibrating the spine, can lead to
injury and back pain. An inactive job or a desk job may also lead
to or contribute to pain, especially if you have poor posture
or sit all day in an uncomfortable chair.
Cigarette smoking: Although smoking
may not directly cause back pain, it increases your risk of developing
low back pain and low back pain with sciatica. (Sciatica is back
pain that radiates to the hip and/or leg due to pressure on a
nerve.) For example, smoking may lead to pain by blocking your
body's ability to deliver nutrients to the discs of the lower
back. Or, repeated coughing due to heavy smoking may cause back
pain. It is also possible that smokers are just less physically
fit or less healthy than nonsmokers, which increases the likelihood
that they will develop back pain. Furthermore, smoking can slow
healing, prolonging pain for people who have had back injuries,
back surgery, or broken bones.
What Are the Causes of Back Pain?
It is important to understand that back pain is a symptom of a medical
condition, not a diagnosis itself. Medical problems that can cause
back pain include the following:
-
Mechanical problems: A mechanical problem
is a problem with the way your spine moves or the way you feel
when you move your spine in certain ways. Perhaps the most common
mechanical cause of back pain is a condition called intervertebral
disc degeneration, which simply means that the discs located between
the vertebrae of the spine are breaking down with age. As they
deteriorate, they lose their cushioning ability. This problem
can lead to pain if the back is stressed. Other mechanical causes
of back pain include spasms, muscle tension, and ruptured discs,
which are also called herniated discs.
Injuries: Spine injuries such as sprains
and fractures can cause either short-lived or chronic pain. Sprains
are tears in the ligaments that support the spine, and they can
occur from twisting or lifting improperly. Fractured vertebrae
are often the result of osteoporosis, a condition that causes
weak, porous bones. Less commonly, back pain may be caused by
more severe injuries that result from accidents and falls.
Acquired conditions and diseases: Many
medical problems can cause or contribute to back pain. They include
scoliosis, which causes curvature of the spine and does not usually
cause pain until mid-life; spondylolisthesis; various forms of
arthritis, including osteoarthritis, rheumatoid arthritis, and
ankylosing spondylitis; and spinal stenosis, a narrowing of the
spinal column that puts pressure on the spinal cord and nerves.
While osteoporosis itself is not painful, it can lead to painful
fractures of the vertebrae. Other causes of back pain include
pregnancy; kidney stones or infections; endometriosis, which is
the buildup of uterine tissue in places outside the uterus; and
fibromyalgia, which causes fatigue and widespread muscle pain.
Infections and tumors: Although they
are not common causes of back pain, infections can cause pain
when they involve the vertebrae, a condition called osteomyelitis,
or when they involve the discs that cushion the vertebrae, which
is called discitis. Tumors, too, are relatively rare causes of
back pain. Occasionally, tumors begin in the back, but more often
they appear in the back as a result of cancer that has spread
from elsewhere in the body.
Although the causes of back pain are usually physical, it is important
to know that emotional stress can play a role in how severe pain is
and how long it lasts. Stress can affect the body in many ways, including
causing back muscles to become tense and painful.
Can Back Pain Be Prevented?
One of the best things you can do to prevent back pain is to exercise
regularly and keep your back muscles strong. Four specific types of
exercises are described in How Is Back Pain Treated?.
All may help you avoid injury and pain. Exercises that increase balance
and strength can decrease your risk of falling and injuring your back
or breaking bones. Exercises such as Tai Chi and yoga – or any
weight-bearing exercise that challenges your balance – are good
ones to try.
Eating a healthy diet also is important. For one thing, eating to
maintain a healthy weight – or to lose weight, if you are overweight
– helps you avoid putting unnecessary and injury-causing stress
and strain on your back. To keep your spine strong, as with all bones,
you need to get enough calcium and vitamin D every day. These nutrients
help prevent osteoporosis, which is responsible for a lot of the bone
fractures that lead to back pain. Calcium is found in dairy products;
green, leafy vegetables; and fortified products, like orange juice.
Your skin makes vitamin D when you are in the sun. If you are not
outside much, you can obtain vitamin D from your diet: almost all
milk and some other foods are fortified with this nutrient. Most adults
don't get enough calcium and vitamin D, so talk to your doctor about
how much you need per day, and consider taking a nutritional supplement
or a multivitamin.
Practicing good posture, supporting your back properly, and avoiding
heavy lifting when you can may all help you prevent injury. If you
do lift something heavy, keep your back straight. Don't bend over
the item; instead, lift it by putting the stress on your legs and
hips.
When Should I See a Doctor for Pain?
In most cases, it is not necessary to see a doctor for back pain
because pain usually goes away with or without treatment. However,
a trip to the doctor is probably a good idea if you have numbness
or tingling, if your pain is severe and doesn't improve with medications
and rest, or if you have pain after a fall or an injury. It is also
important to see your doctor if you have pain along with any of the
following problems: trouble urinating; weakness, pain, or numbness
in your legs; fever; or unintentional weight loss. Such symptoms could
signal a serious problem that requires treatment soon.
Which Type of Doctor Should I See?
Many different types of doctors treat back pain, from family physicians
to doctors who specialize in disorders of the nerves and musculoskeletal
system. In most cases, it is best to see your primary care physician
first. In many cases, he or she can treat the problem. In other cases,
your doctor may refer you to an appropriate specialist.
How Is Back Pain Diagnosed?
Diagnosing the cause of back pain requires a medical history and
a physical exam. If necessary, your doctor may also order medical
tests, which may include x rays.
During the medical history, your doctor will ask questions about
the nature of your pain and about any health problems you and close
family members have or have had. Questions might include the following:
- Have you fallen or injured your back recently?
- Does your back feel better – or hurt worse – when
you lie down?
- Are there any activities or positions that ease or aggravate pain?
- Is your pain worse or better at a certain time of day?
- Do you or any family members have arthritis or other diseases
that might affect the spine?
- Have you had back surgery or back pain before?
- Do you have pain, numbness and/or tingling down one or both legs?
During the physical exam, your doctor may
- watch you stand and walk
- check your reflexes to look for slowed or heightened reflexes,
either of which might suggest nerve problems
- check for fibromyalgia by examining your back for tender points,
which are points on the body that are painful when pressure is applied
to them
- check for muscle strength and sensation
- check for signs of nerve root irritation.
Often a doctor can find the cause of your pain with a physical and
medical history alone. However, depending on what the history and
exam show, your doctor may order medical tests to help find the cause.
Following are some tests your doctor may order:
-
X rays: Traditional x rays use low
levels of radiation to project a picture onto a piece of film
(some newer x rays use electronic imaging techniques). They are
often used to view the bones and bony structures in the body.
Your doctor may order an x ray if he or she suspects that you
have a fracture or osteoarthritis, or that your spine is not aligned
properly.
Magnetic Resonance Imaging (MRI): MRI
uses a strong magnetic force instead of radiation to create an
image. Unlike an x ray, which shows only bony structures, an MRI
scan produces clear pictures of soft tissues, too, such as ligaments,
tendons, and blood vessels. Your doctor may order an MRI scan
if he or she suspects a problem such as an infection, tumor, inflammation,
or pressure on a nerve. An MRI scan, in most instances, is not
necessary during the early phases of low back pain unless your
doctor identifies certain "red flags" in your history
and physical exam. An MRI scan is needed if the pain persists
more than 3-6 weeks, or if your doctor feels there may be a need
for surgical consultation. Because most low back pain goes away
on its own, getting an MRI scan too early may sometimes create
confusion for the patient and the doctor.
Computed Tomography (CT) scan: A CT
scan allows your doctor to see spinal structures that cannot be
seen on traditional x rays. It is a three-dimensional image that
a computer creates from a series of two-dimensional pictures that
it takes of your back. Your doctor may order a CT scan to look
for problems including herniated discs, tumors, or spinal stenosis.
Blood tests: Although blood tests are
not used generally in diagnosing the cause of back pain, your
doctor may order them in some cases. Blood tests that might be
used include the following:
- Complete blood count (CBC), which could point
to problems such as infection or inflammation
- Erythrocyte sedimentation rate (also called sed rate),
a measure of inflammation that may suggest infection. The presence
of inflammation may also suggest some forms of arthritis or,
in rare cases, a tumor.
It is important to understand that medical tests alone may not diagnose
the cause of back pain. In fact, experts say that up to 90 percent
of all MRI scans of the spine show some type of abnormality, and sometimes
the x rays and CT scans of people without pain show problems. Similarly,
even some healthy pain-free people can have elevated sed rates.
Only with a medical history and exam - and sometimes medical tests
- can a doctor diagnose the cause of back pain. Many times, the precise
cause of back pain is never known. In these cases, it may be comforting
to know that most back pain gets better whether or not you find out
what is causing it.
What Is the Difference Between Acute and Chronic
Pain?
Pain that hits you suddenly – after falling from a ladder,
being tackled on the football field, or lifting a load that is just
too heavy, for example – is acute pain. Acute pain comes on
quickly and often leaves just as quickly. To be classified as acute,
pain should last no longer than 6 weeks. Acute pain is the most common
type of back pain.
Chronic pain, on the other hand, may come on either quickly or slowly,
and it lingers a long time. In general, pain that lasts more than
3 months is considered chronic. Chronic pain is much less common than
acute pain.
How Is Back Pain Treated?
Treatment for back pain generally depends on what kind of pain you
experience: acute or chronic.
-
Acute Back Pain: Acute back pain usually
gets better on its own and without treatment, although you may
want to try acetaminophen, aspirin, or ibuprofen to help ease
the pain. Perhaps the best advice is to go about your usual activities
as much as you can with the assurance that the problem will clear
up. Getting up and moving around can help ease stiffness, relieve
pain, and have you back doing your regular activities sooner.
Exercises are not usually advisable for acute back pain, nor
is surgery.
Chronic Back Pain: Treatment for chronic
back pain falls into two basic categories: the kind that requires
an operation and the kind that does not. In the vast majority
of cases, back pain does not require surgery. Doctors will almost
always try nonsurgical treatments before recommending surgery.
In a very small percentage of cases – when back pain is
caused by a tumor, an infection, or a nerve root problem called
cauda equina syndrome, for example – prompt surgery is necessary
to ease the pain and prevent further problems.
Following are some of the more commonly used treatments for chronic
back pain.
Nonoperative treatments
-
Hot or cold: Hot or cold packs –
or sometimes a combination of the two – can be soothing
to chronically sore, stiff backs. Heat dilates the blood vessels,
improving the supply of oxygen that the blood takes to the back
and reducing muscle spasms. Heat also alters the sensation of
pain. Cold may reduce inflammation by decreasing the size of blood
vessels and the flow of blood to the area. Although cold may feel
painful against the skin, it numbs deep pain. Applying heat or
cold may relieve pain, but it does not cure the cause of chronic
back pain.
Exercise: Although exercise is usually
not advisable for acute back pain, proper exercise can help ease
chronic pain and perhaps reduce its risk of returning. The following
four types of exercise are important to general physical fitness
and may be helpful for certain specific causes of back pain:
-
Flexion: The purposes of flexion exercises,
which are exercises in which you bend forward, are to 1) widen
the spaces between the vertebrae, thereby reducing pressure
on the nerves; 2) stretch muscles of the back and hips; and
3) strengthen abdominal and buttock muscles. Many doctors
think that strengthening the muscles of the abdomen will reduce
the load on the spine. One word of caution: If your back
pain is caused by a herniated disc, check with your doctor
before performing flexion exercises because they may increase
pressure within the discs, making the problem worse.
Extension: With extension exercises, you
bend backward. They may minimize radiating pain, which is
pain you can feel in other parts of the body besides where
it originates. Examples of extension exercises are leg lifting
while lying prone and raising the trunk while lying prone.
The theory behind these exercises is that they open up the
spinal canal in places and develop muscles that support the
spine.
Stretching: The goal of stretching exercises,
as their name suggests, is to stretch and improve the extension
of muscles and other soft tissues of the back. This can reduce
back stiffness and improve range of motion.
Aerobic: Aerobic exercise is the type that
gets your heart pumping faster and keeps your heart rate elevated
for a while. For fitness, it is important to get at least
30 minutes of aerobic (also called cardiovascular) exercise
three times a week. Aerobic exercises work the large muscles
of the body and include brisk walking, jogging, and swimming.
For back problems, you should avoid exercise that requires
twisting or vigorous forward flexion, such as aerobic dancing
and rowing, because these actions may raise pressure in the
discs and actually do more harm than good. In addition, avoid
high-impact activities if you have disc disease. If back pain
or your fitness level makes it impossible to exercise 30 minutes
at a time, try three 10-minute sessions to start with and
work up to your goal. But first, speak with your doctor or
physical therapist about the safest aerobic exercise for you.
Medications: A wide range of medications
are used to treat chronic back pain. Some you can try on your
own. Others are available only with a doctor's prescription. The
following are the main types of medications used for back pain.
-
Analgesics: Analgesic medications are those
designed specifically to relieve pain. They include over-the-counter
acetaminophen (Tylenol1)
and aspirin, as well as prescription narcotics, such as oxycodone
with acetaminophen (Percocet) or hydrocodone with acetaminophen
(Vicodin). Aspirin and acetaminophen are the most commonly
used analgesics; narcotics should only be used for a short
time for severe pain or pain after surgery. People with muscular
back pain or arthritis pain that is not relieved by medications
may find topical analgesics helpful. These creams, ointments,
and salves are rubbed directly onto the skin over the site
of pain. They use one or more of a variety of ingredients
to ease pain. Topical analgesics include such products as
Zostrix, Icy Hot, and Ben Gay.
1 Brand names
included in this booklet are provided as examples only, and
their inclusion does not mean that these products are endorsed
by the National Institutes of Health or any other Government
agency. Also, if a particular brand name is not mentioned,
this does not mean or imply that the product is unsatisfactory.
NSAIDs: Nonsteroidal anti-inflammatory drugs (NSAIDs)2
are drugs that relieve pain and inflammation, both of which
may play a role in some cases of back pain. Aspirin, ibuprofen,
naproxen, and naproxen sodium are examples of NSAIDs. They
are often the first type of medication used. All NSAIDs work
similarly: by blocking substances called prostaglandins that
contribute to inflammation and pain. However, each NSAID is
a different chemical, and each has a slightly different effect
on the body.
Some NSAIDS are available over the counter, while more than
a dozen others, including a subclass called COX-2 inhibitors,
are available only with a prescription.
All NSAIDS can have significant side effects, and for unknown
reasons, some people seem to respond better to one NSAID than
another. Any person taking NSAIDS regularly should be monitored
by a doctor.
2Warning:
NSAIDs can cause stomach irritation or, less often, they can
affect kidney function. The longer a person uses NSAIDs, the
more likely he or she is to have side effects, ranging from
mild to serious. Many other drugs cannot be taken when a patient
is being treated with NSAIDs because NSAIDs alter the way
the body uses or eliminates these other drugs. Check with
your health-care provider or pharmacist before you take NSAIDs.
Also, NSAIDs sometimes are associated with serious gastrointestinal
problems, including ulcers, bleeding, and perforation of the
stomach or intestine. People over age 65 and those with any
history of ulcers or gastrointestinal bleeding should use
NSAIDs with caution.
Other Medications: Muscle relaxants and
certain antidepressants have also been prescribed for chronic
back pain, but their usefulness is questionable.
Traction: Traction involves using pulleys
and weights to stretch the back. The rationale behind traction
is to pull the vertebrae apart to allow a bulging disc to slip
back into place. Some people experience pain relief while in traction,
but that relief is usually temporary. Once traction is released,
the stretch is not sustained and back pain is likely to return.
There is no scientific evidence that traction provides any
long-term benefits for people with back pain.
Corsets and braces: Corsets and braces
include a number of devices, such as elastic bands and stiff supports
with metal stays, that are designed to limit the motion of the
lumbar spine, provide abdominal support, and correct posture.
While these may be appropriate after certain kinds of surgery,
there is little, if any, evidence that they help treat chronic
low back pain. In fact, by keeping you from using your back muscles,
they may actually cause more problems than they solve by causing
lower back muscles to weaken from lack of use.
Behavioral modification: Developing
a healthy attitude and learning to move your body properly while
you do daily activities – particularly those involving heavy
lifting, pushing, or pulling – are sometimes part of the
treatment plan for people with back pain. Other behavior changes
that might help pain include adopting healthy habits, such as
exercise, relaxation, and regular sleep, and dropping bad habits,
such as smoking and eating poorly.
Injections: When medications and other
nonsurgical treatments fail to relieve chronic back pain, doctors
may recommend injections for pain relief. Following are some of
the most commonly used injections, although some are of questionable
value:
-
Nerve root blocks: If a nerve is inflamed
or compressed as it passes from the spinal column between
the vertebrae, an injection called a nerve root block may
be used to help ease the resulting back and leg pain. The
injection contains a steroid medication and/or anesthetic
and is administered to the affected part of the nerve. Whether
the procedure helps or not depends on finding and injecting
precisely the right nerve.
Facet joint injections: The facet joints
are those where the vertebrae connect to one another, keeping
the spine aligned. Although arthritis in the facet joints
themselves is rarely the source of back pain, the injection
of anesthetics or steroid medications into facet joints is
sometimes tried as a way to relieve pain. The effectiveness
of these injections is questionable. One study suggests
that this treatment is overused and ineffective.
Trigger point injections: In this procedure,
an anesthetic is injected into specific areas in the back
that are painful when the doctor applies pressure to them.
Some doctors add a steroid medication to the injection. Although
the injections are commonly used, researchers have found that
injecting anesthetics and/or steroids into trigger points
provides no more relief than "dry needling," or
inserting a needle and not injecting a medication.
Prolotherapy: One of most talked-about procedures
for back pain, prolotherapy is a treatment in which a practitioner
injects a sugar solution or other irritating substance into
trigger points along the periosteum (the tough, fibrous tissue
covering the bones) to trigger an inflammatory response that
promotes the growth of dense, fibrous tissue. The theory behind
prolotherapy is that such tissue growth strengthens the attachment
of tendons and ligaments whose loosening has contributed to
back pain. As yet, studies have not verified the effectiveness
of prolotherapy. The procedure is used primarily by chiropractors
and osteopathic physicians.
Complementary and alternative treatments:
When back pain becomes chronic or when medications and other conventional
therapies do not relieve it, many people try complementary and
alternative treatments. While such therapies won't cure diseases
or repair the injuries that cause pain, some people find them
useful for managing or relieving pain. Following are some of the
most commonly used complementary therapies.
-
Manipulation: Spinal manipulation refers
to procedures in which professionals use their hands to mobilize,
adjust, massage, or stimulate the spine or surrounding tissues.
This type of therapy is often performed by osteopathic doctors
and chiropractors. It tends to be most effective in people
with uncomplicated pain and when used with other therapies.
Spinal manipulation is not appropriate if you have a medical
problem such as osteoporosis, spinal cord compression, or
inflammatory arthritis (such as rheumatoid arthritis) or if
you are taking blood-thinning medications such as warfarin
(Coumadin) or heparin (Calciparine, Liquaemin).
Transcutaneous Electrical Nerve Stimulation (TENS):
TENS involves wearing a small box over the painful area that
directs mild electrical impulses to nerves there. The theory
is that stimulating the nervous system can modify the perception
of pain. Early studies of TENS suggested it could elevate
the levels of endorphins, the body's natural pain-numbing
chemicals, in the spinal fluid. But subsequent studies
of its effectiveness against pain have produced mixed results.
Acupuncture: This ancient Chinese practice
has been gaining increasing acceptance and popularity in the
United States. It is based on the theory that a life force
called Qi (pronounced chee) flows through the body along certain
channels, which if blocked can cause illness. According to
the theory, the insertion of thin needles at precise locations
along these channels by practitioners can unblock the flow
of Qi, relieving pain and restoring health.
Although few Western-trained doctors would agree with the
concept of blocked Qi, some believe that inserting and then
stimulating needles (by twisting or passing a low-voltage
electrical current through them) may foster the production
of the body's natural pain-numbing chemicals, such as endorphins,
serotonin, and acetylcholine.
A consensus panel convened by the National Institutes of
Health (NIH) in 1997 concluded that there is clear evidence
this treatment is effective for some pain conditions, including
postoperative dental pain. Although there is less convincing
evidence to support using acupuncture for back pain and some
other pain conditions, the panel concluded that acupuncture
may be effective when used as part of a comprehensive treatment
plan for low back pain, fibromyalgia, and several other conditions.
Acupressure: As with acupuncture, the theory
behind acupressure is that it unblocks the flow of Qi. The
difference between acupuncture and acupressure is that no
needles are used in acupressure. Instead, a therapist applies
pressure to points along the channels with his or her hands,
elbows, or even feet. (In some cases, patients are taught
to do their own acupressure.) Acupressure has not been
well studied for back pain.
Rolfing: A type of massage, rolfing involves
using strong pressure on deep tissues in the back to relieve
tightness of the fascia, a sheath of tissue that covers the
muscles, that can cause or contribute to back pain. The theory
behind rolfing is that releasing muscles and tissues from
the fascia enables the back to properly align itself. So
far, the usefulness of rolfing for back pain has not been
scientifically proven.
Operative treatments
Depending on the diagnosis, surgery may either be the first treatment
of choice – although this is rare – or it is reserved
for chronic back pain for which other treatments have failed. If you
are in constant pain or if pain reoccurs frequently and interferes
with your ability to sleep, to function at your job, or to perform
daily activities, you may be a candidate for surgery.
In general, there are two groups of people who may require surgery
to treat their spinal problems. People in the first group have chronic
low back pain and sciatica, and they are often diagnosed with a herniated
disc, spinal stenosis, spondylolisthesis, or vertebral fractures with
nerve involvement. People in the second group are those with only
predominant low back pain (without leg pain). These are people with
discogenic low back pain (degenerative disc disease), in which discs
wear with age. Usually, the outcome of spine surgery is much more
predictable in people with sciatica than in those with predominant
low back pain.
Some of the diagnoses that may need surgery include:
-
Herniated discs: a potentially painful
problem in which the hard outer coating of the discs, which are
the circular pieces of connective tissue that cushion the bones
of the spine, are damaged, allowing the discs' jelly-like center
to leak, irritating nearby nerves. This causes severe sciatica
and nerve pain down the leg. A herniated disc is sometimes called
a ruptured disc.
Spinal stenosis: the narrowing of the
spinal canal, through which the spinal cord and spinal nerves
run.
It is often caused by the overgrowth of bone caused by osteoarthritis
of the spine. Compression of the nerves caused by spinal stenosis
can lead not only to pain, but also to numbness in the legs and
the loss of bladder and/or bowel control. Patients may have difficulty
walking any distances and may also have severe pain in their legs
along with numbness and tingling.
Spondylolisthesis: a condition in which
a vertebra of the lumbar spine slips out of place. As the spine
tries to stabilize itself, the joints between the slipped vertebra
and adjacent vertebrae can become enlarged, pinching nerves as
they exit the spinal column. Spondylolisthesis may cause not only
low back pain but severe sciatica leg pain.
Vertebral fractures: fractures caused
by trauma to the vertebrae of the spine or by crumbling of the
vertebrae resulting from osteoporosis. This causes mostly mechanical
back pain, but it may also put pressure on the nerves, creating
leg pain.
Discogenic Low Back Pain (Degenerative Disc Disease):
Most people's discs degenerate over a lifetime, but in some, this
aging process can become chronically painful, severely interfering
with their quality of life.
Following are some of the most commonly performed back surgeries:
-
For herniated discs:
-
Laminectomy/discectomy: In this
operation, part of the lamina, a portion of the bone on the
back of the vertebrae, is removed, as well as a portion of
a ligament. The herniated disc is then removed through the
incision, which may extend two or more inches.
Microdiscectomy: As with traditional
discectomy, this procedure involves removing a herniated disc
or damaged portion of a disc through an incision in the back.
The difference is that the incision is much smaller and the
doctor uses a magnifying microscope or lenses to locate the
disc through the incision. The smaller incision may reduce
pain and the disruption of tissues, and it reduces the size
of the surgical scar. It appears to take about the same time
to recuperate from a microdiscectomy as from a traditional
discectomy.
Laser surgery: Technological advances
in recent decades have led to the use of lasers for operating
on patients with herniated discs accompanied by lower back
and leg pain. During this procedure, the surgeon inserts a
needle in the disc that delivers a few bursts of laser energy
to vaporize the tissue in the disc. This reduces its size
and relieves pressure on the nerves. Although many patients
return to daily activities within 3 to 5 days after laser
surgery, pain relief may not be apparent until several weeks
or even months after the surgery. The usefulness of laser
discectomy is still being debated.
For spinal stenosis:
-
Laminectomy: When narrowing of
the spine compresses the nerve roots, causing pain and/or
affecting sensation, doctors sometimes open up the spinal
column with a procedure called a laminectomy. In a laminectomy,
the doctor makes a large incision down the affected area of
the spine and removes the lamina and any bone spurs, which
are overgrowths of bone, that may have formed in the spinal
canal as the result of osteoarthritis. The procedure is major
surgery that requires a short hospital stay and physical therapy
afterwards to help regain strength and mobility.
For spondylolisthesis:
-
Spinal fusion: When a slipped vertebra
leads to the enlargement of adjacent facet joints, surgical
treatment generally involves both laminectomy (as described
above) and spinal fusion. In spinal fusion, two or more vertebrae
are joined together using bone grafts, screws, and rods to
stop slippage of the affected vertebrae. Bone used for grafting
comes from another area of the body, usually the hip or pelvis.
In some cases, donor bone is used.
Although the surgery is generally successful, either type
of graft has its drawbacks. Using your own bone means surgery
at a second site on your body. With donor bone, there is a
slight risk of disease transmission or rejection. In recent
years, a new development has eliminated those risks for some
people undergoing spinal fusion: proteins called bone morphogenic
proteins are being used to stimulate bone generation, eliminating
the need for grafts. The proteins are placed in the affected
area of the spine, often in collagen putty or sponges.
Regardless of how spinal fusion is performed, the fused area
of the spine becomes immobilized.
For vertebral osteoporotic fractures3:
-
Vertebroplasty: When back pain
is caused by a compression fracture of a vertebra due to osteoporosis
or trauma, doctors may make a small incision in the skin over
the affected area and inject a cement-like mixture called
polymethyacrylate into the fractured vertebra to relieve pain
and stabilize the spine. The procedure is generally performed
on an outpatient basis under a mild anesthetic.
3 Used only if standard care, rest, corsets/braces,
analgesics fail.
Kyphoplasty: Much like vertebroplasty,
kyphoplasty is used to relieve pain and stabilize the spine
following fractures due to osteoporosis. Kyphoplasty is a
two-step process. In the first step, the doctor inserts a
balloon device to help restore the height and shape of the
spine. In the second step, he or she injects polymethyacrylate
to repair the fractured vertebra. The procedure is done under
anesthesia, and in some cases it is performed on an outpatient
basis.
For Discogenic Low Back Pain (Degenerative Disc Disease)
-
Intradiscal electrothermal therapy (IDT):
One of the newest and least invasive therapies for low back
pain involves inserting a heating wire through a small incision
in the back and into a disc. An electrical current is then
passed through the wire to strengthen the collagen fibers
that hold the disc together. The procedure is done on an outpatient
basis, often under local anesthesia. The usefulness of
IDT is debatable.
Spinal fusion: When the degenerated
disc is painful, the surgeon may recommend removing it and
fusing the disc to help with the pain. This fusion can be
done through the abdomen, a procedure known as anterior lumbar
interbody fusion, or through the back, called posterior fusion.
Theoretically, fusion surgery should eliminate the source
of pain; the procedure is successful in about 60 to 70 percent
of cases. Fusion for low back pain or any spinal surgeries
should only be done as a last resort, and the patient should
be fully informed of risks.
Disc replacement: When a disc is
herniated, one alternative to a discectomy – in which
the disc is simply removed – is removing it and replacing
it with a synthetic disc. Replacing the damaged one with an
artificial one restores disc height and movement between the
vertebrae. Artificial discs come in several designs. Although
doctors in Europe had performed disc replacement for more
than a decade, the procedure had been experimental in the
United States until the Food and Drug Administration approved
the Charite artificial disc (http://www.fda.gov/cdrh/mda/docs/p040006.htm)
for use.
What Kind of Research Is Being Done?
The National Institute of Arthritis and Musculoskeletal and Skin
Diseases (NIAMS) is currently supporting a number of studies to better
understand and treat back pain. Goals of current research include
the following:
-
To compare the effectiveness of surgery versus nonsurgical
treatment for low back pain. Although the percentage
of people having spinal surgery in the United States has increased
sharply over time, there is not much information on whether back
surgery is better than nonoperative treatments. One study is comparing
the most commonly used surgical treatments to the most commonly
used nonoperative treatments for three common back problems: herniated
discs of the lumbar spine, spinal stenosis, and spinal stenosis
from spondylolisthesis. The study, being conducted at 12 medical
centers, will follow patients for at least 24 months after treatment
to determine the medical- and cost-effectiveness of treatments.
To identify the best treatments for certain low back
pain patients. Just as certain treatments are effective
for some back problems and not others, the same treatment may
be effective for some people and not others – even if those
people have the same medical problem. Researchers at several centers
will study more than 3,000 patients who have one of three common
causes of back pain – herniated discs, spinal stenosis,
and spondylolisthesis – and who respond well to specific
treatments. Extensive testing and surveys will allow doctors to
identify the best treatments for these patients.
To test the effectiveness of lumbar fusion and other
treatments for disc-derived pain. Discogenic pain
is low back pain due to the wearing away of a disc between the
vertebrae. While treatment for this condition is often lumbar
spinal fusion, its effectiveness, as well as that of other treatments,
has not been established. A new study will compare the results
of spinal fusion with those of nonsurgical care for patients with
similar disc degeneration. Researchers will also try to find out
1) what distinguishes people who choose surgery from those who
do not; 2) the consequences of common complications of spinal
fusion surgery and how often they occur; 3) what predicts a good
response to surgical therapy but not to other treatments; and
4) what are the characteristics and outcomes of patients who have
repeat back surgery for this condition.
To measure the frequency of complications in lumbar
fusion surgery. Lumbar spinal fusion is a commonly
performed procedure for several back problems, including disc
degeneration, spondylolisthesis, spinal stenosis, and scoliosis,
but the procedure can have complications. A new study will follow
1,000 people who have spinal fusion for one of these diagnoses
to find out 1) how often complications occur after surgery, 2)
how the rates of specific serious complications vary with different
types of lumbar fusion, 3) the consequences of specific types
of complications, and 4) the characteristics of treatments or
patients that predict particularly severe complications. The information
will help doctors better assess the benefits versus the risks
of the procedure.
To better understand the relationship between the
loss of motor control and low back pain. Compared
to people without back problems, those with low back pain show
losses in motor control, including problems with trunk muscle
response and posture. Some researchers believe that losses in
motor control may predispose people to falls that result in back
pain. Other researchers think losses in motor control may result
from damage sustained by tissue during a fall. To explore the
relationship between motor control loss and back pain, scientists
will study varsity athletes to determine whether poor motor control
of the lumbar spine increases the risk of low back injury. They
will also study changes in the lumbar spine motor control of people
with low back pain after they complete rehabilitation programs
that emphasize motor control training.
To develop and evaluate a psychosocial program for
people with acute low back pain. Acute low back
pain is a common problem that affects people's abilities to work
and function, and it contributes to high health care costs. There
are few studies, however, that prove whether or not a treatment
truly reduces limitation and prevents the recurrence of pain.
One new project will develop a program to enhance the social support
and self-efficacy of people with acute low back pain. After developing
and testing the program, researchers will evaluate its effectiveness
by comparing the results of 160 participants with those of 160
people receiving usual care.
To evaluate the nervous system mechanisms of low
back pain. Scientists think that when a disc ruptures,
material leaking from its jelly-like filling leads to inflammation
and the release of chemicals that irritate cells within the spinal
canal. Scientists believe that the effects of these chemicals
on the nerve endings in discs and adjacent tissue lead to low
back pain, while the effects on dorsal nerve roots lead to sciatica.
One study will test these ideas using a variety of techniques.
A better understanding of pain mechanisms related to herniated
discs will allow researchers to develop better treatments.
To evaluate an Internet-based patient education program.
Patient education can play an important role in managing back
pain. Yet taking part in an educational program can be difficult
and time-consuming for some people, particularly if they live
far from an area where such a program is offered. This study,
conducted with patients recruited from Silicon Valley employers
and the Internet, will test the effectiveness of an Internet-based
education program. Participants will receive a book and videotape,
and they will interact with other program participants through
a moderated Internet discussion group. Patient assessments will
also be conducted through the Internet.
For More Information
-
National Institute of Arthritis and Musculoskeletal and Skin
Diseases (NIAMS)
Information Clearinghouse
National Institutes of Health
1 AMS Circle
Bethesda, MD 20892-3675
Phone: 301-495-4484
Toll Free: 877-22-NIAMS (226-4267)
TTY: 301–565–2966
Fax: 301-718-6366
Email: NIAMSinfo@mail.nih.gov
Website: http://www.niams.nih.gov
-
National Institute of Neurological Disorders and Stroke (NINDS)
NIH Neurological Institute
P.O. Box 5801
Bethesda, MD 20824
Phone: 301–496–5751
Toll Free: 800–352–9424
TTY: 301–468–5981
Website: http://www.ninds.nih.gov
-
National Center for Complementary and Alternative Medicine
National Institutes of Health
P.O. Box 7923
Gaithersburg, MD 20898
Phone: 301-519-3153
Toll Free: 888-644-6226
TTY: 866-464-3615
Fax: 866-464-3616
Email: info@nccam.nih.gov
Website: http://nccam.nih.gov
-
Agency for Health Care Research and Quality Clearinghouse
540 Gaither Road
Rockville, MD 20850
Phone: 301–427–1364
Website: http://www.ahcpr.gov
-
Clearinghouse for Occupational Safety and Health Information
4676 Columbia Parkway
Cincinnati, Oh 513–533–8326
Phone: 800–356–4674
Website: http://www.cdc.gov/niosh/homepage.html
-
American Academy of Orthopaedic Surgeons (AAOS)
P.O. Box 2058
Des Plaines, IL 60017
Toll Free: 800-824-BONE (2663)
Email: pemr@aaos.org
Website: http://www.aaos.org
-
North American Spine Society (part of AAOS)
22 Calendar Court 2nd Floor
LaGrange, IL 60525
Phone: 877–SPINE-DR
Toll Free: 877-SpineDr (877-774-6337)
Email: info@spine.org
Website: http://www.spine.org
-
American College of Rheumatology (ACR)
1800 Century Place, Suite 250
Atlanta, GA 30345-4300
Phone: 404-633-3777
Fax: 404-633-1870
Website: http://www.rheumatology.org
-
Arthritis Foundation
P.O. Box 7669
Atlanta, GA 30357-0669
Phone: 404-872-7100
Toll Free: 800-283-7800
Website: http://www.arthritis.org
-
American Chiropractic Association
1701 Clarendon Boulevard
Arlington, VA 22209
Toll Free: 800–986–4636
Website: http://www.amerchiro.org
-
American Osteopathic Association
142 East Ontario Street
Chicago, Il 60611
Phone: (312) 202-8000
Toll Free: (800) 621-1773
Website: http://www.osteopathic.org/
Glossary
-
Acupuncture – an ancient Chinese practice
that involves inserting thin needles at various sites on the body
to relieve pain or influence other body processes. Today, doctors
use acupuncture for problems as diverse as addiction, morning
sickness, and back pain.
Acute pain – the most common type of back
pain. Acute pain often begins suddenly – after a fall or
injury, for example – and lasts for 6 weeks or less.
Analgesics – medications designed to relieve
pain. Analgesics used for back pain include those that are available
by prescription or over-the-counter and those made to be taken
orally or rubbed onto the skin.
Ankylosing spondylitis – a form of arthritis
that affects the spine, the sacroiliac joints, and sometimes the
hips and shoulders. In severe cases, the joints of the spine fuse
and the spine becomes rigid.
Cauda equina syndrome – a condition in
which the nerves that control the bowels and bladder are pinched
as they leave the spine. Unless treated promptly, the condition
can lead to the loss of bowel and/or bladder function.
Cervical spine – the upper portion of
the spine closest to the skull. It is composed of seven vertebrae.
Chronic pain – the least common type of
back pain. Chronic pain may begin either quickly or slowly; it
generally lasts for 3 months or more.
Disc – circular pieces of cushioning tissue
situated between each of the spine's vertebrae. Each disc has
a strong outer cover and a soft jelly-like filling.
Discectomy – the surgical removal of a
herniated disc. A discectomy can be performed in a number of different
ways, such as through a large incision in the spine or through
newer, less-invasive procedures using magnifying microscopes,
x rays, small tools, and even lasers.
Facet joints – the joints where the vertebrae
of the spine connect to one another. Arthritis of the facet joints
is believed to be an uncommon cause of back pain.
Fibromyalgia – a condition of widespread
muscle pain, fatigue, and tender points on the body. Fibromyalgia
is one cause of low back pain.
Herniated disc – a potentially painful
problem in which the hard outer coating of the disc is damaged,
allowing the disc's jelly-like center to leak and cause irritation
to adjacent nerves.
Intradiscal electrothermal therapy (IDT) –
a treatment for herniated discs in which a wire is inserted into
the disc through a small incision in the back. An electrical current
is then passed through wire to modify and strengthen the collagen
fibers that hold the disc together.
Kyphoplasty – a procedure for vertebral
fractures in which a balloon-like device is inserted into the
vertebra to help restore the height and shape of the spine and
a cement-like substance is injected to repair and stabilize it.
Laminectomy – the surgical removal of
the lamina (the back of the spinal canal) and spurs inside the
canal that are pressing on nerves within the canal. The procedure
is a major surgery requiring a large incision and a hospital stay.
Lumbar spine – the lower portion of the
spine. It is composed of five vertebrae.
Osteoarthritis – a disease in which the
cartilage that cushions the ends of the bones at the joints wears
away, leading to pain, stiffness, and bony overgrowths, called
spurs. It is the most common form of arthritis and becomes more
likely with age.
Osteoporosis – a condition in which the
bones become porous and brittle, and break easily.
Prolotherapy – a treatment for back pain
in which a practitioner injects a sugar solution or other irritating
substance into trigger points along the periosteum (tough, fibrous
tissue covering the bones) to trigger an inflammatory response
that promotes the growth of dense, fibrous tissue. The theory
behind prolotherapy is that such tissue growth strengthens the
attachment of tendons and ligaments whose loosening has contributed
to back pain.
Rolfing – a type of massage that uses
strong pressure on deep tissues in the back to relieve tightness
of the fascia (a sheath of tissue that covers the muscles) that
can cause or contribute to back pain.
Rheumatoid arthritis – a disease that
occurs when the body's immune system attacks the tissue that lines
the joints, leading to joint pain, inflammation, instablity, and
misshapen joints.
Sacroiliac joints – the joints where the
spine and pelvis attach. The sacroiliac joints are often affected
by types of arthritis referred to as spondyloarthropathies.
Sciatica – pain felt down the back and
outer side of the thigh. The usual cause is a herniated disc,
which is pressing on a nerve root.
Scoliosis – a condition in which the spine
curves to one side as a result of congenital malformations, neuromuscular
disorders, injury, infection, or tumors.
Spinal fusion – the surgical joining of
two more vertebrae together, usually with bone grafts and hardware.
The resulting fused vertebrae are stable but immobile. Spinal
fusion is used as a treatment for spondylolisthesis, scoliosis,
herniated discs, and spinal stenosis.
Spinal stenosis – the narrowing of the
spinal canal (through which the spinal cord runs), often by the
overgrowth of bone caused by osteoarthritis of the spine.
Spondyloarthropathy – a form of arthritis
that primarily affects the spine and sacroiliac joints.
Spondylolisthesis – a condition in which
a vertebra of the lumbar (lower) spine slips out of place.
Transcutaneous Electrical Nerve Stimulation (TENS)
– a treatment designed to relieve pain by directing mild
electrical impulses to nerves in the painful area of the body.
Vertebrae – the individual bones that
make up the spinal column.
Vertebroplasty – a minimally invasive
surgical procedure that involves injecting a cement-like mixture
into a fractured vertebra to relieve pain and stabilize the spine.
Acknowledgments
The NIAMS gratefully acknowledges the assistance of James Kang, M.D.,
University of Pittsburgh, PA; Jeffrey Katz, M.D., Brigham and Women's
Hospital, Boston, MA; William Lauerman, M.D., Georgetown University,
Washington, DC; and James Panagis, M.D., M.P.H., NIAMS, NIH, Bethesda,
MD, in the preparation and review of this booklet. Special thanks
also go to the other individuals who reviewed this publication and
provided valuable assistance.
The mission of the National Institute of Arthritis and Musculoskeletal
and Skin Diseases (NIAMS), a part of the Department of Health and
Human Services' National Institutes of Health (NIH), is to support
research into the causes, treatment, and prevention of arthritis and
musculoskeletal and skin diseases; the training of basic and clinical
scientists to carry out this research; and the dissemination of information
on research progress in these diseases. The National Institute of
Arthritis and Musculoskeletal and Skin Diseases Information Clearinghouse
is a public service sponsored by the NIAMS that provides health information
and information sources. Additional information can be found on the
NIAMS Web site.
For Your Information
This publication contains information about medications used to treat
the health condition discussed here. When this booklet was printed,
we included the most up-to-date (accurate) information available.
Occasionally, new information on medication is released.
For updates and for any questions about any medications you are taking,
please contact the U.S. Food and Drug Administration at:
-
U.S. Food and Drug Administration
Toll Free: 888-INFO-FDA (888-463-6332)
Website: http://www.fda.gov/
This booklet is not copyrighted. Readers are encouraged to duplicate
and distribute as many copies as needed.
Additional copies of this booklet are available from
-
National Institute of Arthritis and Musculoskeletal and Skin
Diseases (NIAMS)
Information Clearinghouse
National Institutes of Health
1 AMS Circle
Bethesda, MD 20892-3675
Phone: 301-495-4484
Toll Free: 877-22-NIAMS (226-4267)
TTY: 301–565–2966
Fax: 301-718-6366
Email: NIAMSinfo@mail.nih.gov
Website: http://www.niams.nih.gov
|

